As one of the nurses and I were just discussing, in the hospital, and especially in the ICU, things can change so quickly...for the better but unfortunately, also for the worse. This past Thursday, Rowan had a pretty okay day. They were able to pull off a lot of fluid via dialysis, he did not require any blood or platelet transfusions, and we were able to stop his insulin drip. Friday, things started to change. He went back on iv pressors to keep his BP up, back on insulin, was pale and lethargic, had a high respiratory rate, high heart rate, and was requiring blood sugar checks (finger or toe pokes) every 30 minutes all day, as well as blood pressure checks (arm cuff squeezes) every 5 minutes all day...you heard me right ... every 5 minutes. He was getting sicker, but he was also getting more and more miserable...and tired. By Saturday morning, he was on 2 pressors (one, at a higher level than he has been this entire stay), a much higher drip of insulin. He received 2 red blood cell transfusions, 2 rapid fluid boluses, stress dosing steroids, and had an ART line placed, but he seemed to be holding his own. He was only on 1-2 L of nasal cannula oxygen for comfort during the day, and was switched to High Flow nasal cannula overnight.
Sunday, the switch was flipped. He was switched over to BiPAP, received 4 platelet infusions, 3 red blood cell infusions and 2 albumin infusions in 24 hours.
Early Sunday morning as respiratory therapy was attempting to fit him for a smaller BiPAP mask Rowan was fighting me. He kept telling me, "I don't need this, I don't need this, let me prove it to you right now. I can breathe on my own." I explained to him that we were doing it for his own good, because it was taking too much for him to breathe on his own now and keep his sats up. He continued to argue with me as they switched the mask over. During that transition, Rowan started to desat...significantly. He stared at me, wide eyed at first, and started panicking. He said, through very labored breathing, ""I'm sorry Mommy, I'm sorry Mommy, you're right... I can't breathe. I can't breathe. I can't..." And with that he started to close his eyes. There were 6-7 of us in the room at the time. I stepped back to let respiratory therapy and the nurses take charge of the situation. Then, I heard one of the statements you never want to hear while in the ICU with your child. A nurse grabbed Rowan by the face, looked him in the eyes and said "Stay with me Rowan. Stay with me, okay?", as the RT worked fervently to refit his BiPAP and stabilize his breathing. He quickly recovered and I came back closer to the bed, to be by his side. Rowan looked over at me with tears in his eyes, and said "Ok, Ok, Ok, I'm sorry. Ok Mommy". The scare made him realize how much he needed help. He now knew that he needed to be on the BiPAP, and he was scared enough to do so willingly the rest of the day. The crazy part, was that he kept apologizing for it. He felt bad for fighting us. He was more concerned with having offended us, than he was himself. I guess I shouldn't be surprised.
Throughout the day, his respiratory requirements continued to increase. He needed more and more fi02 settings, and had lower and lower sats. It was such a trying day. By the late afternoon, the doctors were rounding by his room every 30 minutes to an hour, and warned me that he may be close to needing to intubated. At first I did not want them to do that. Neither did Rowan. It is a difficult decision to make when he was still able to talk to me and still knew what was going on, etc. But his vitals and his blood gas labs started to prove that he really needed the break. Sometime around 1:00 am he could no longer keep his sats above 80s, his respiratory rate was in the 60s, and he was very uncomfortable, working extremely hard to breathe. I looked at the doctor with tears in my eyes and said "Okay, yes, I see that he needs it."
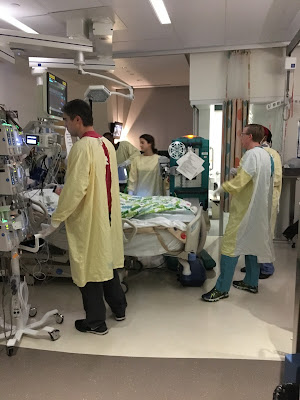
Rowan's ICU room quickly started to fill and change shape. They had such a well oiled machine working though. I wanted to stay because it is torture being outside, wondering how things are going the whole time they are working on him. They allowed me to be in the room, and I chose a corner to stand in. I wanted to be near, but did not want a front row seat. I will not describe every detail, because it is an undesirable and unimaginable experience, and honestly, I may not be words to adequately paint the picture.
What I will say, is that Rowan is intubated and remains on the vent right now. We were up until 5 am in the morning to make sure he settled in to the vent settings and stabilized. And as always, I was truly impressed with this child's ability to remain calm, grateful and agreeable during such a difficult scenario. He signed "thank you" to the doctors and nurses as he drifted off to sleep, under the sedation.
But now, I wanted to share his last words before intubation. Rowan of course warned the doctor, "Remember, I need more propofol than the normal person." I didn't want to be his last words before intubation, so I prompted him, saying "Every Day...?" and he answered me, "I will get stronger." I said, "I love you Rowan." and he mouthed, "I love you too." I thought that would be it...but then Rowan sweetly called out to the room, "Okay, I hope nobody is wearing blue gloves in here." We all chuckled. Then they got to work. Rowan did desat, and he did have to be manually bagged a few times while getting him attached to the correct mask. The person placing the tube stood at the head of Rowan's bed and warned her attending, "This isn't gong to be easy. He's so swollen. I don't have a good view." The attending concurred. The next moments, felt like hours, while they sedated, prepped, attempted, paused to bag, and then performed the intubation. No mother should ever have to witness such a traumatic event. And hearing the attending tell the fellow, "You have 60 seconds"...so intense.
In the end, Rowan was successfully intubated, and was placed on the ventilator with some pretty high settings. The goal and the hope is that his lungs and breathing will heal and recover with this respiratory break. He has remained stable during the day today. He arouses, and he is in pain, but his work of breathing is much improved on the vent. I thank God for the amazing team of nurses and doctors that he has aligned for us. I learn more and more each day, not just about medicine, but about true compassion and dedication. These people have saved my son...again. We are forever in your debt.







God bless you and this amazing child. Sending you love and prayers.
ReplyDeleteMy heart goes out to you.....he is such a special little guy ...it always amazes me that kids in these instances can have such a good sense of humor....the blue gloves...wow...just to let you know my husband and I are praying for Rowan and you too....lots of love, hugs and prayers....God Bless you!!!!
ReplyDeleteRowan hold on buddy this amazing team of medical staff are fighting to save your life with Gods hand right there. You are so loved and so many prayers from around the world 🌎 our God hears them all. My prayers for for you continue lord I ask you please remove the fluids being contained in Rowan's body work on the problems at hand now lord one issue at a time make this baby whole again he still is so strong and and fighting He's proven many times what a fighter he is. His family has been so strong the faith they have comes from you Lord. I ask for my Christmas prayers is to bless this beautiful family with positive good and only good from this day forward for healing to begin let Rowan give his family a gift they need. In the name of Jesus Amen!
ReplyDeleteI'm GODS name Amen
DeleteHe's a strong lil warrior...
ReplyDeleteWe are paying for him n the family mom...
You all got this...
Always in my thoughts n prayers...
Prayers of comfort for Rowan and his family. Thank you for sharing his story. God Bless.
ReplyDeletePrayers for this precious child of God and for his amazing family.
ReplyDeleteBless his heart. He does look peaceful now. Prayers that God will heal and rest him so he can get off the vent soon.
ReplyDeleteRowan, Carrie and family, you are all in my prayers. I believe that you will come out of this eventually, and oh what a testimony you will have. Through your pain and your faith in Jesus, others will find hope in the midst of their trials. Still I am sorry that you have to go through all this pain. It has to be so scary.so many people are praying for you. Where two or more are gathered Jesus is right there with you. You are never alone. Praying that this all pass soon and for you to be home healthy and happy. Love you Rowan!
ReplyDeleteYour family is in our prayers...
ReplyDeleteJust praying that this rest is what Rowan needs right now and things start to improve. We are praying in New Jersey for our little warrior! We are also praying and sending hugs to his family and all those wonderful doctors, nurses, techs taking care of sweet Rowan.
ReplyDeleteI don't know you or your family, but what an incredible and inspiring story of love and fortitude. Stay strong. Lots of prayers going out to you.
ReplyDeleteI think of you both everyday , Praying constantly for complete healing ! Keep Fighting little man !!
ReplyDeleteMom stay strong and know we are thinking of you!
Fighting back the pain and tears just from your words. Prayers to Rowan and family. That's all I've got ...there is no words.
ReplyDeleteCarrie and Brian and kids and Rowan hold on to God and know God is not done! And in the eye of the storm God is always in control!!!luv u all!
ReplyDeletePraying for you all now... xxo
ReplyDeleteMy heart goes out to Rowan and I pray for Rowan, you, and your family daily.
ReplyDeleteAll I want... is to see those beautiful blue eyes of his, smiling! What a beautiful child you have. Carrie, you are such a strong person. I pray for you guys daily. We're all praying for you. Hang in there. Keep up the faith!
ReplyDeleteI have been following Rowans and your family's story for awhile .I am in Aww of him and you !He is the strongest Lil boy I know ( I feel like I know him ) his strength and courage is amazing ! You are a awesome mother Carrie !! Please keep your head up and know You have a lot of people there for you !!I Love Rowan & you both!! Btw my fb name is Tammy Nicole
ReplyDeleteGod bless you always Rowan! You are a TRUE inspiration to many sweet child. Please keep fighting sweet one, I feel as if the whole world should know you! Many have not had the blessing to meet or know you. Keep fighting because I know people will see GOD in you and they themselves need that. May people in this world have lost their faith in God and I know that in just meeting you and getting to hear your story, people will change for the better. I pray everyday for you and for your momma! God bless your parents, please God be their strength! We love you Rowan!
ReplyDeleteCarrie,
ReplyDeleteI don't know you, but my husband Jim Connolly went to HS with you. Over the past few years he has mentioned you and little Rowan's fight. He gives me updates from time to time, and more recently has been forwarding me your blog. He is not an emotional guy, but he sure is attached to Rowan and his fight.
First I just wanted to tell you we are praying for you and your family.
Second you are an amazing mother! Rowan is blessed to have you.
Third Rowan is awe-inspiring little boy. His spirit, willingness to fight and wisdom beyond his years is a blessing.
Sending lots of prayers and love to you both.
Keeping little Rowan in my prayers.. May God heal his little body soon. Stay strong mommy. Love you little Rowan.
ReplyDeleteKansas
Praying for Rowan, stay strong little man, the whole world is praying for you!
ReplyDeleteFight on Rowan! <3 from Keller, TX
ReplyDeleteSo so sad prayers on the way xxxxx
ReplyDeleteI prayed that today would never come, sadly it did... RIP sweet boy. To your Mom, Im so sorry, this isnt fair :( *hugs*
ReplyDelete